What is Vagus Nerve Stimulation (VNS)?
LISTEN TO THIS ARTICLE:
What it is
Vagus Nerve Stimulation (VNS) started out as a treatment for epilepsy. It found new purpose after patients who had received the device for seizure control reported mood improvements, especially for depression.
VNS treats Major Depressive Disorder by sending periodic electrical signals to the brain via the vagus nerve.
Who needs it
In 2005, the U.S. Food and Drug Administration cleared it as an adjunctive treatment for chronic, recurrent major depressive disorder in patients who had failed to respond to at least four antidepressants. The depression must be severe and have lasted at least two years. “Adjunctive” treatments should only be used in combination with medication or other forms of well-established treatment. Vagus Nerve Stimulation is appropriate for patients who have “treatment-resistant depression”, which affects 15-33% of depressed people.
How Vagus Nerve Stimulation works
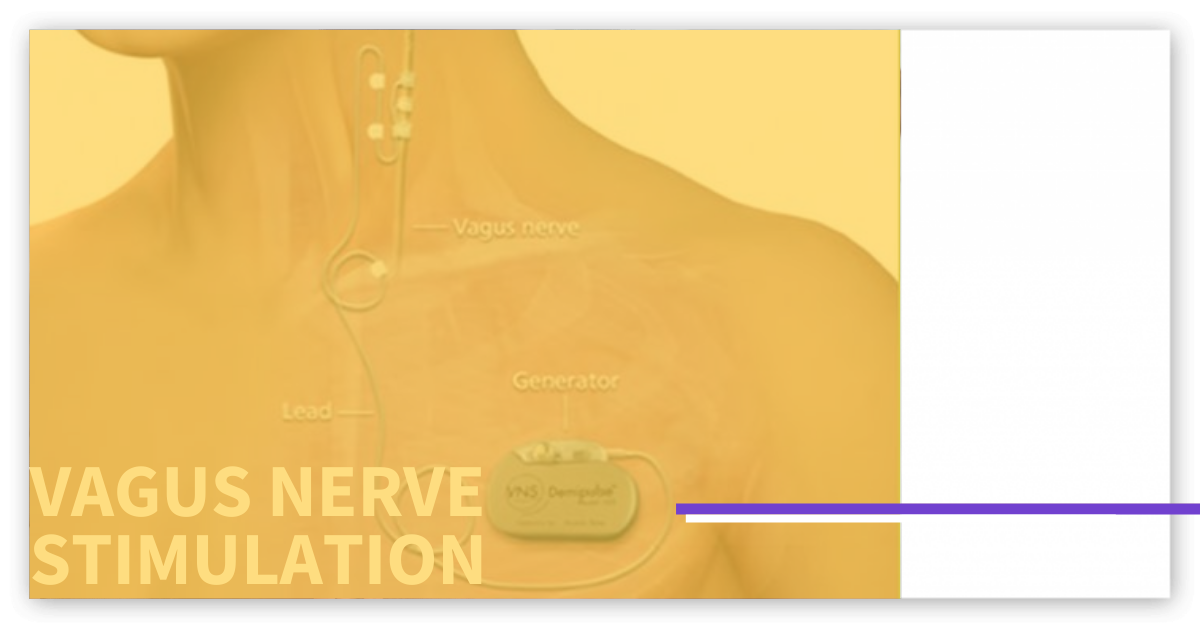
First, a neurosurgeon implants the watch-sized device under the skin of the left upper chest. Then, they run a wire to the left vagus nerve in the neck. This is a minor surgical procedure that takes about one hour and does not require an overnight stay in the hospital.
A significant majority of the fibers making up the vagus nerve carry information towards the brain and connect to areas involved in mood regulation and depression. Brain imaging shows that stimulation of these fibers increases release of neurotransmitters such as norepinephrine and serotonin in these brain areas. This mechanism is similar to the effects of antidepressant medications.
Where to go
After a surgeon places the device, the patient follows up with a psychiatrist during several weekly sessions. The psychiatrist wirelessly calibrates the device to send electrical signals lasting 30 to 90 seconds to the vagus nerve every 5 to 10 minutes. The doctor adjusts the strength and frequency of pulses to minimize side effects.
What to expect
Depending on how doctors assessed patients for depression, 22 to 32% respond at least partially to Vagus Nerve Stimulation. Between 15% and 23% achieve remission of their depression in 12 months. It can take a matter of weeks to months before patients notice benefits.
Patients who receive a VNS device should expect to continue taking medications as it is not meant to be a standalone treatment.
What could happen
Patients can experience stimulation-related side effects, such as voice changes, cough, and headache. Side effects related to stimulation tend to decrease with time as the body develops tolerance. If the side effects ever become intolerable, the patient can turn the device off by holding a magnet over the skin where the implant is placed.
The surgery has very rare side effects like permanent voice changes and facial muscle weakness. This only happens if other nerves in the neck become damaged during the procedure.
Because Vagus Nerve Stimulation treatment for depression is relatively new, your insurance may not cover it, or, if they do, it may require a prior authorization. Prescribing and calibrating the device requires specific training and experience. Not every psychiatrist will offer it, so patients may have to travel to find one who does. Patients considering this treatment should contact their insurance companies directly.


 Learn
Learn ID Symptom
ID Symptom Find Help
Find Help